The NHS screens people for various conditions and diseases throughout our lives, from pregnancy to old age.
Screening stops people from becoming ill and saves lives.
Watch the video or read on below to see how it works and the vital impact it has.
How it works
Screening looks for early signs of illness or disease through some straightforward tests on blood or cell samples, scans, or x-rays.
The earlier these risk factors are identified, the sooner they can be treated, either stopping the condition from developing or significantly reducing the impact on a person’s health.
Why the NHS screens for certain conditions
There are several factors that the NHS will consider when deciding which conditions to screen for.
Firstly, it must be easily detectable in its earliest stages with simple tests that produce clear and accurate results.
Secondly, early treatment can remove or significantly reduce the chances of the disease developing.
And finally, the screening process isn’t harmful to patients, and any discomfort is outweighed by the potential benefit it brings.
Conditions that fit these criteria are part of the NHS programme include bowel, breast, and cervical cancer and abdominal aortic aneurysm (a condition when a major blood vessel swells and ruptures).
Measuring impact through statistics
Some of the most telling – and linked – statistics around these conditions are the number of cases and deaths recorded every year and the number of people who take up the offer of screening.
There is clear evidence that when screening rates go up, the number of cases and deaths reduces, clearly showing the impact of screening.
There are also figures about the percentage of preventable cases – meaning that had the person been screened and treated, the condition would not have developed.
The purpose of sharing these figures is to highlight that lives are lost that could have been saved through screening, especially with conditions where screening rates are decreasing.
Let’s look at some diseases’ incidence and the impact of screening.
Breast cancer
One in seven women will get breast cancer throughout their lives.
Every year, over 55,000 new cases are recorded in this country, and over 11,500 people die due to breast cancer.
Twenty-three per cent of these cases – nearly 1 in 4 – could have been prevented by screening.
Regular screening is offered to all women starting at age 50 and continuing until they are 71.
If you are registered with a GP practice, you will automatically be sent a letter inviting you to book an appointment.
Despite the effectiveness of the screening programme, the number of people taking up the invitation has decreased in recent years.
In 2006, nearly three-quarters of women – 74.8% – regularly attended breast screenings. By 2021, this figure had fallen to 62.8%. This change amounts to around 400,000 fewer women being regularly screened.
Remembering that 23% of all breast cancer cases can be prevented, it’s easy to calculate that of the more than 11,500 breast cancer deaths each year, more than 2,500 could be avoided.
Abdominal Aortic Aneurysm
An Abdominal Aortic Aneurysm – or AAA – is when a swelling or bulge in the aorta, the main blood vessel running from your heart to your tummy, ruptures.
This is a very dangerous condition. Eight in ten people who suffer an AAA will die before they get to hospital. The disease accounts for around 5,000 deaths in this country every year.
Screening plays such an essential part because people rarely experience symptoms of AAA other than an actual rupture. By this time, it is often too late.
Men are much more likely to develop AAA – incidence is six times higher than women. Smokers, however, are up to fifteen times more at risk.
Because of the much higher incidence in males, all men are invited to a screening when they turn 65.
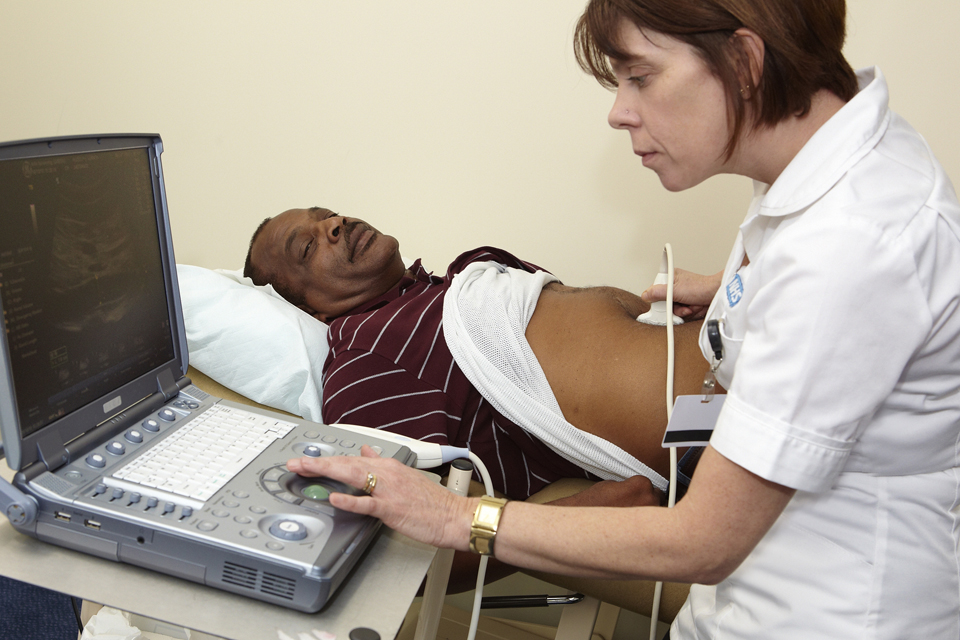
The screening process involves an ultrasound of the abdomen, measuring the width of the aorta and looking for any swelling or bulges. It takes about 10 minutes and is painless.
Around one in ninety-two men who are screened will have some degree of bulge or swelling. Depending on the severity, treatments can range from making lifestyle changes to slow the growth, or surgery.
Because of the lack of symptoms and the sudden severity of a rupture, screening is an essential tool in saving lives.
Cervical Cancer
While the number of annual cases (3,200) and deaths (850) due to cervical cancer are much smaller than some other cancers, one significant statistic jumps out.
Nearly all cases of cervical cancer are preventable. 99.8% of cases and deaths could be avoided through screening.
Despite this being a condition that could almost be wiped out with comprehensive screening, fewer women and people with cervixes are getting regularly screened.
In 2011, the uptake was 73.7%. Ten years later, in 2021, that had fallen to 68%.
That means that 3 in every ten women and people with a cervix are not getting regular screened.
Screening begins at age 25, continuing every three years until age 64. The highest incidence of cervical cancer is in the age group 30-34 years old.
Increasing the number of people who attend cervical screening appointments is something the NHS invests considerable time into because the impact of screening is so significant.

Bowel Cancer
Like cervical cancer, screening could prevent a very high percentage of bowel cancer cases.
Nearly 43,000 cases are recorded every year, and more than 16,500 deaths.
Over half of these cases – fifty-four per cent – could be avoided with screening.
The risk of bowel cancer increases significantly with age, peaking in people in the 85-90 bracket.
That’s why testing starts for men and women at 60 and continues at regular intervals of 2 years.
The screening is carried out with a ‘test at home’ kit that people are sent in the post. It is a simple and effective test.
Since 2010, the number of people regularly screened for bowel cancer has increased from 50.1% to over 70% in 2021.
Directly linked to this is a decrease in deaths recorded over the same time. Twelve per cent fewer people die due to bowel cancer than a decade ago.
